Surgical Dermatology
Nobody performs more surgical procedures on the skin than dermatologists. Nobody.
Board-certified dermatologists are highly trained skin surgeons performing thousands of procedures per year on nearly every body surface. From simple biopsies to complex surgical repairs, board-certified dermatologists have the experience and training to deliver optimal outcomes.
Regardless of whether you require removal of a benign growth or excision and repair of a large facial skin cancer, Clarus Dermatology should be your first stop. We will discuss medical and surgical options for treatment so you can select the one that best fits your care goals. Often, our physicians will perform the operation and reconstruction, but frequently we work with highly-vetted sub-specialists in otolaryngology, radiation oncology and plastic surgery to deliver the care that you need.

Nobody performs more surgical procedures on the skin than dermatologists. Nobody.
Board-certified dermatologists are highly trained skin surgeons performing thousands of procedures per year on nearly every body surface. From simple biopsies to complex surgical repairs, board-certified dermatologists have the experience and training to deliver optimal outcomes.
Regardless of whether you require removal of a benign growth or excision and repair of a large facial skin cancer, Clarus Dermatology should be your first stop. We will discuss medical and surgical options for treatment so you can select the one that best fits your care goals. Often, our physicians will perform the operation and reconstruction, but frequently we work with highly-vetted sub-specialists in otolaryngology, radiation oncology and plastic surgery to deliver the care that you need.
Dermatologists = Skin cancer experts
We are in the midst of an epidemic of skin cancer. If you or a loved one develops skin cancer of any type, we urge you to meet with our dermatologists. Our comprehensive approach involves three steps:
- Evaluation of the tumor.All dermatologists are trained as skin pathologists. As such, we are in a unique position to determine the best treatment options for you given the location, type, and subtype, of your tumor. We often review your pathology slides if we did not perform the diagnostic biopsy in-house.In contrast to many other practices, all Clarus dermatologists personally review each of their pathology specimens to ensure agreement with the outside pathologist’s assessment. This allows for superior “clinico-pathologic correlation” which leads to better outcomes for you. For example, often skin cancer can be treated by more conservative treatment strategies after review of the tumor itself.
- Evaluation of the patient. Before we choose the answers, we ask the questions. We put the particulars of your skin cancer into the context of your overall goals. How will your other medical conditions influence the healing process? Does your family history play a role? Are you healthy enough to undergo a major surgery with reconstruction? These are some of the questions that your dermatologist will consider when discussing treatment options with you.
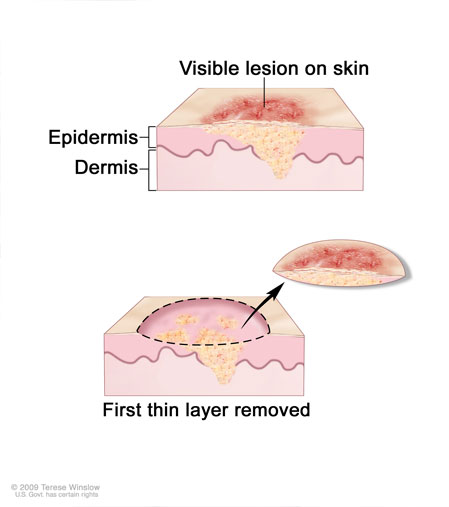
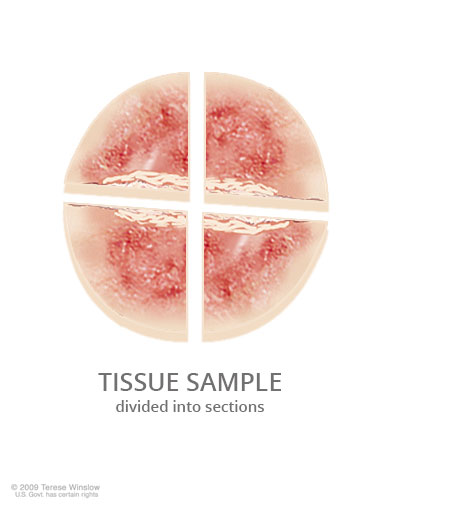
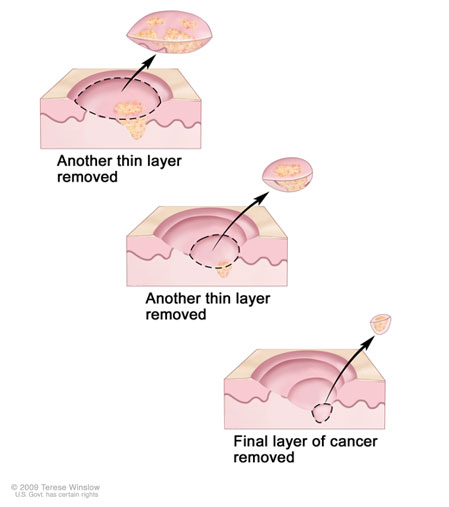
- Evaluation of your options. Although aggressive types of skin cancer surgery, like Mohs surgery, can be considered for many tumors, they often are not aligned with the patient’s care goals. We work with you to ensure that our recommendations respect your wishes.
- Completion of care. Once we have evaluated the tumor, the patient and his/her care goals we can proceed with treatment. Throughout this step you will be in the hands of an expertly trained, board-certified dermatologist and the entire Clarus care team.
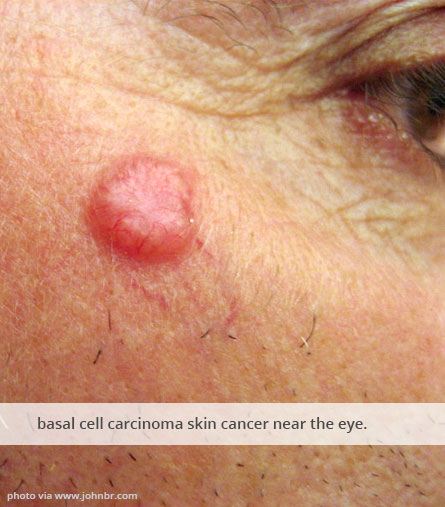
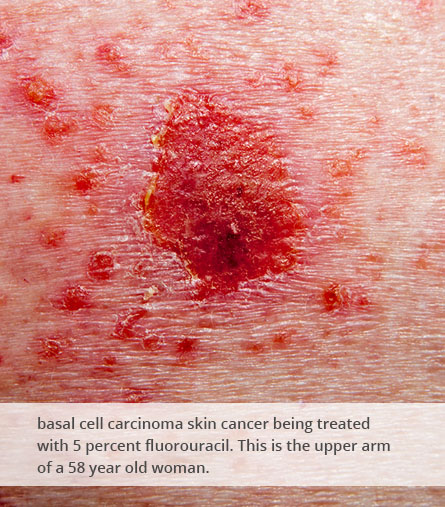
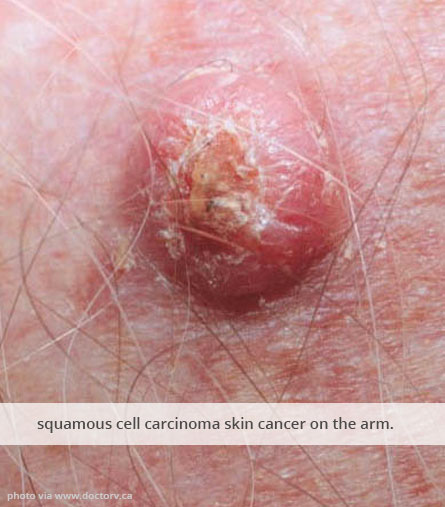
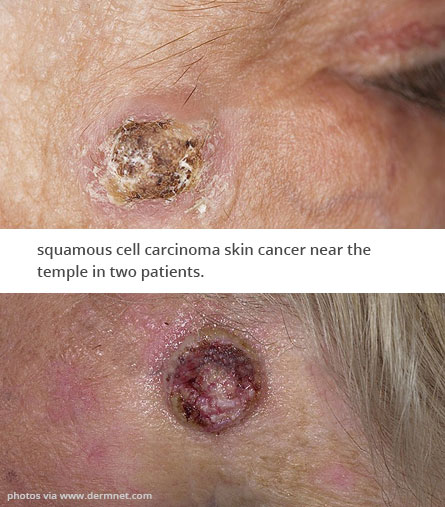
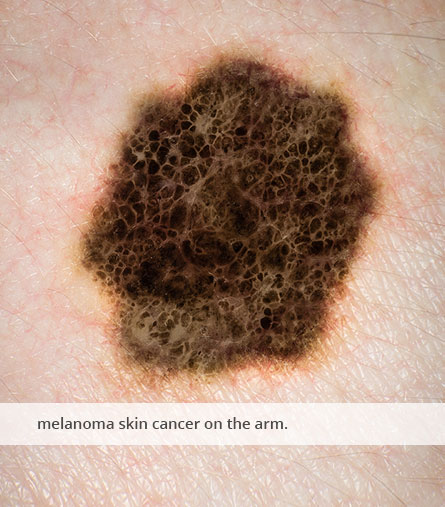
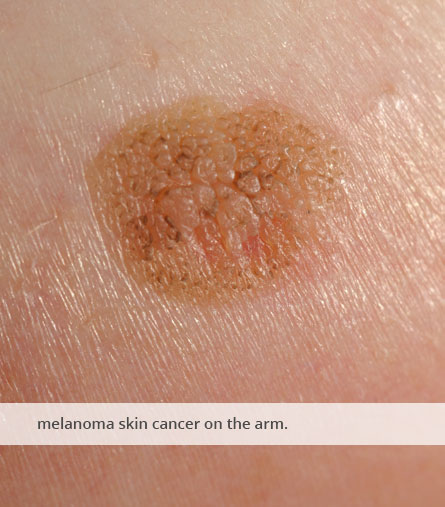
About Skin Cancer
Frequently asked questions for surgical patients
What surgical services do you provide?
We provide a wide range of services including, but not limited to the following:
-Skin surgery on all body surfaces, including destruction of benign and malignant growths, excisional surgery, Mohs Micrographic Surgery, skin biopsy, scar revision including injection and resurfacing
Why can’t I schedule directly for surgery?
It is very important that we have adequate time to discuss the risks, benefits and alternatives of a given surgical approach with you before we schedule your procedure. Careful review of your existing pathology, medical history and care goals will determine the most appropriate treatment. Infrequently, additional biopsies must be performed prior to making a treatment recommendation.
Your pre-operative clinic visit ensures that our dermatologists have all of the information they need regarding your skin cancer, your medical history and your treatment goals to schedule the appropriate surgical procedure. It will also give you a chance to ask questions you might have about your condition and your treatment plan.
How should I prepare for my surgery?
While it’s not always easy to do when dealing with the time before a surgery, our best advice is simple: in a word: relax. In many cases, you will not need to make major changes during this time, but may have just a few simple instructions that you will need to follow in the hours just before your procedure.
Generally, most medications can be safely continued through your surgery, including blood thinners such as coumadin and aspirin. Refer to our detailed pre-operative instructions online for the procedure you’ll be having, or in the letter you received in the mail.
Who do I call if I have problems after my surgery?
Surgical complications do occur, but we are there for you 24/7. You will receive your surgeon’s cell-phone number at the time of surgery. We are there for you to ensure your post-operative course is as smooth as possible.